We are trained to think that autism is a permanent condition where our only options are to improve function through repetitive behavioral management therapies and pharmaceutical symptom suppression. Is this the best we can do for our children?
I have been documenting stories of full reversal, remission, recovery (pick your word) from autism for nearly 20 years. Documenting Hope has published two peer-reviewed papers in the medical literature (here and here) documenting the full reversal of autism in three children. Documenting Hope has collected dozens and dozens of autism healing stories on our website and YouTube channel.
Do you know what didn’t recover these children?
ABA.
It might have been used to help families manage behaviors, improve function, and get through the day, but it isn’t the mechanism that healed these children’s very dysregulated bodies. Yet this is the only autism therapy or service that is widely covered by Medicaid or health insurance in all 50 states. And for some families, it is only partially covered, and they are left penniless just trying to pay for a therapy that some would argue is only marginally beneficial.
If you don’t have a child with autism, you probably aren’t familiar with ABA, so let’s start with a brief explanation of what it is, where it came from, and what it is trying to accomplish.
What Is ABA?
The most common form of therapy for autism is called applied behavior analysis or ABA. ABA has its roots in the psychological science of operant conditioning (how behavior is shaped by consequences) and was further developed in the 1960s by psychologists who saw autism as a fixed disorder but one that could improve through behavioral training. The idea behind ABA is that rewarding certain behaviors, or providing positive reinforcement, will encourage children to repeat desired behaviors. The earliest forms of ABA involved putting children through a set of pre-established tasks with lots of repetition, removed from a naturalistic environment. Newer forms of ABA have evolved that are based on play and other activities that are part of children’s normal lives. Early forms of ABA also used punishment for undesirable behaviors in addition to positive reinforcement of desired behaviors. But let’s not go there for right now.
While some more updated forms of ABA, like Pivotal Response Treatment, look to reward behaviors in a more naturalistic or play-based context, they are still focused on rewarding or reinforcing “correct” behaviors instead of understanding the origins of the “incorrect” or “problematic” behavior. It is not biology-first or root-cause oriented.
While ABA will not help your child reverse or overcome his autism diagnosis, it can help you manage behaviors and improve certain functions. Will ABA help you and your child get through the day? Yes. Accomplish necessary tasks? Yes. Give you respite while your child is working with the therapist? Yes.
Is there value to parents whose children receive ABA therapy? Yes, absolutely. But if you are a parent who wants to see your child reach his or her full potential or heal the underlying medical and developmental dysfunctions that contribute to symptoms of autism or “problematic behaviors,” ABA is not your therapy. Sadly, for many parents, this is their only choice. This needs to change.
The focus of ABA is on changing behaviors, especially “problem behaviors” or behavior deficits. Behaviors are taught and reinforced in an effort to increase functional skills or reduce barriers to learning. ABA therapists and technicians are not physicians, and they do not get training in the underlying medical reasons that might be responsible for the “unwanted” behaviors. They generally do not assess biomedical causes as contributors to unwanted behaviors. More holistically oriented ABA therapists would certainly understand the role that nutrition, sleep, and exercise/movement might play in a child’s behaviors, but they may not understand that the child they are working with is dealing with very severe medical issues that manifest as behaviors. Some of these severe medical issues include: chronic inflammation, gut dysbiosis, mitochondrial dysfunction, mold toxicity, heavy metal toxicity, metabolic disease, nervous-system dysregulation, and more. Here is why this matters: Overlooking these important medical issues in favor of “training” a child into a functional behavior could actually result in the unintended traumatization of a child.
Unintended Traumatization Via Behavioral Reinforcement
Before diving into what will likely be a very controversial topic, I want you to understand something very important. My critique of ABA as a therapeutic model is not the same thing as a critique of the therapists or the parents who utilize this therapy. On the whole, the therapists working with children with autism are caring, patient and professional and truly want to see each child thrive. The parents who enroll their children in ABA therapy programs are doing what they have been told is the “gold standard” evidence-based treatment for autism, and they will probably see some tangible improvement in the quality of life for the family and in the daily functioning for the child.
But just because good and well-intended people are using this therapy does not mean it is the best strategy to help a child with autism overcome his or her greatest challenges. It is a strategy that should ideally be employed after a child’s body becomes healthy and regulated enough to comfortably receive behavioral training.
Now that we have established all that, here is a very concrete illustration of how traditional ABA might result in the unintended traumatization of a child. Avoiding eye contact (reduced eye gaze, eye aversion, sideways glancing) is one of the most common features of autism and has been described as the most reliably replicated early predictor of ASD. If a child is unable to make eye contact, the ABA therapist might practice a routine where he or she holds something the child desires (such as bubbles, spinning toys or a toy train) right near their own face, mouth or eyes so the child is encouraged to look toward the therapist’s face (a proxy for eye contact). If the child glances at the therapist’s face, he is immediately rewarded and will be rewarded even more the longer the gaze is held. This activity may be couched within a play-based setting. On the outside, it may seem like a positive and encouraging way to interact with the child. The therapist is engaged, smiling, warm, caring and enthusiastic, so what could possibly be wrong with this approach?
While ABA therapists do this training from a place of compassion, understanding that this may be a difficult and stressful task for these children, many do not fully understand the biology and physiology behind the lack of eye contact. If they did, they would want to address the underlying root causes of eye aversion before ever trying to force it (even if gently and compassionately) through positive reinforcement strategies.
Eye Aversion, the Nervous System and Why ABA Can Be Dysregulating and Stressful
Lack of eye contact can reflect neurological dysregulation, brain inflammation, sensory or emotional overload, discomfort, or developmentally rooted vision problems. Developmental optometrists/neuro-optometrists and functional neurologists among other root cause oriented clinicians understand that the reason that the child is doing this is not because they “won’t” make eye contact, it is because they can’t comfortably make eye contact or they can’t safely execute the steps required to make eye contact. Averting eye contact is an adaptive behavior for a child seeking the feeling of safety.
This is an important distinction. The child’s behavior (eye aversion) isn’t because they “won’t” do it (viewed as the “problematic behavior”). It is because they “can’t comfortably or safely” do it. The child will not make eye contact because they may be dealing with a dysregulated nervous system or a neurological or neurodevelopmental condition like a binocular vision dysfunction, convergence insufficiency, visual motion sensitivity or other similar dysfunction. These are sophisticated neurological and vision diagnoses that are often completely missed in children with autism.
What it means experientially for this child, though, is that eye contact may feel disorienting, dizzying or overwhelming. What’s more, children with autism are experiencing nervous system dysregulation at baseline and may be in a state of “fight or flight” (commonly documented in children with ASD). Being asked to integrate the visual and emotional stimulus of making eye contact can further enhance the feeling of threat or danger. A crude analogy might be that forcing a dysregulated child with autism to make eye contact during an ABA session is like asking a child in a state of fear to watch a clip from a horror movie and rewarding them to do so.
How Does Making Eye Contact Worsen Nervous-System Dysregulation?
Looking at faces requires visual decoding and emotional interpretation. For a child who has a dysregulated nervous system and is stuck in “fight or flight,” eye contact might feel unsafe or too complex to be able to handle. Imaging studies show that direct gaze can be associated with heightened amygdala activity (indicating fear or lack of safety) and subcortical activation (rapid emotional reaction). Reduced eye contact may function as a way to reduce over-arousal or perceived threat. Children with autism are just trying to create a state of safety for themselves.
As has been well-established by Dr. Robert Naviaux at UCSD, children with autism live in a state of chronic threat or danger activation. Dr. Naviaux has published groundbreaking work on a function called the cell danger response, an adaptive mechanism our cells default to as a result of past or present threats to the safety of the cell. The threats could be from toxins, emotions, infections, inflammation and more. His groundbreaking research has found that cellular threat signaling remains chronically active in children with autism. This is chronic danger biology, hypervigilance, and sympathetic dominance of the autonomic nervous system (“fight or flight”).
Direct gaze is not a simple visual act; it is a high-load social, emotional, and sensory event.
It asks an individual in chronic danger biology to take on more threat and more danger.
So, they don’t.
They look sideways because peripheral vision is calmer and requires less emotional intensity than direct gaze. Looking sideways is a safer way for them to handle visual demands.
Let’s stop right here and really think about what I have just said. ABA is rewarding children (sometimes with candy) for doing something that makes them feel dizzy, disoriented, overwhelmed and unsafe. I can already hear the ABA therapists saying: “But we do this in a safe, gradual and gentle fashion, never pushing them beyond what they can handle.”
I understand that, but when working with a child with autism (many of whom cannot communicate with speech or even intentional gestures), this is akin to a coercive form of exposure therapy, a popular technique employed by psychologists to help people overcome fears and phobias by re-introducing something in little bits that terrifies someone.
Increasingly, trauma-informed therapists are critiquing exposure therapy because it can risk overwhelming or retraumatizing the nervous system if underlying trauma and neurobiology is not adequately addressed and the individual does not consent to the exposure. Without consent and without addressing the underlying nervous-system dysregulation first, the individual cannot feel fully safe and in control. Many children with autism do not have the opportunity to consent to the ABA behavioral techniques, nor are they provided with nervous-system regulation techniques or strategies prior to beginning the behavioral training. Many are nonspeakers and do not have a way to communicate the dysregulation and feelings of danger caused by the ABA techniques and practices. To be fair, there are some more progressive ABA practitioners who do intentionally practice co-regulation prior to beginning a session, but this is the exception, not the rule, and it isn’t necessarily taught as a foundational principle in BCBA (board certified behavior analyst) training, nor is it taught to RBTs (Registered Behavior Technician), the technicians hired to do much of the one-on-one work in an ABA clinic. There are some BCBAs and RBTs who are actively calling for a collaborative model of care where a functional, root-cause medical approach would be applied before, or in conjunction with, behavioral training to ultimately improve outcomes in ABA. Here is an article written by such a technician.
Ultimately, if a child’s underlying trauma (cell danger response, neuroinflammation, nervous-system dysregulation, sensory sensitivity) is not addressed first, forced or coercive behaviors reinforce sympathetic nervous system dominance (“fight or flight”) and exacerbate cell-danger biology. So, while the intentions are pure, some forms of ABA may be unknowingly and unintentionally traumatizing children in a trade-off for behavioral compliance and what is perceived as improved functioning.
This raises important questions about the ethics of strategies used in ABA and creates an urgency for us to rethink autism therapy.
How ABA Misses the Mark on Speech and Communication
There are other concerning aspects of ABA that are rising to the surface, thanks to the growth of spelling and communication techniques for nonspeakers and those who cannot produce reliable speech or written language (estimated at around 30-40% of individuals with autism).
For decades, nonspeakers diagnosed with autism were erroneously presumed to be of low intelligence and capacity for learning. This was presumed by teachers, parents and therapists alike. Spelling and communication techniques such as RPM, Spellers Method and S2C were developed to help individuals use motor function they do have intact — gross-motor function — to support communication efforts. Because these individuals lacked the motor function necessary to be able to reliably produce speech, written language or typical communication, they were presumed to be developmentally “stuck” at the same stage as toddlers, with only pre-reliable speech. In reality, their intellect and cognition were as developed as their neurotypical peers, but no one knew! Inability to speak isn’t an inborn feature of autism. It is the outward symptom expression of a body that is experiencing apraxia, mitochondrial dysfunction, bioenergetic dysfunction, neuroinflammation, and other underlying physiological features that impact the development of speech.
Speech is among the most metabolically expensive functions in our bodies. If a body is stuck in danger biology and is not metabolically healthy (as can be assessed by this test and this test and this one, too), it cannot afford to shunt energy to speech and socialization. Speech is one of the first functions to fail when the brain must conserve energy and prioritize survival. This is because spontaneous speech requires enormous integration across sensory, cognitive, emotional, respiratory, and fine-motor systems. A nonspeaker may understand far more than they can motorically express. Cell-danger biology and mitochondrial dysfunction can help explain why some nonspeaking autistic individuals lose reliable access to speech: not because they necessarily lack language or thought, but because the brain-body system does not have the metabolic stability, sensory regulation, and motor-planning capacity needed to execute speech consistently.
Imagine if you were a brilliant 18-year-old nonspeaker diagnosed with autism who was cognitively capable of doing college-level calculus, learning foreign languages, and interpreting complex poetry (not to mention have crushes, love pop music, enjoy spending time with friends and other normal teenage stuff) but you have motor planning and execution impairments so significant that you cannot form speech, or reliably gesture to communicate your needs. Now imagine an ABA therapist giving you mind-numbing repetitive tasks that feel like they are made for 2- and 3-year-olds because it is part of your therapeutic program to improve function and daily life. Can you imagine how maddening that would be? This is happening to many nonspeakers today. Shouldn’t we spend our time and effort working on making every nonspeaker metabolically healthy? Shouldn’t we focus on improving cellular health, reducing inflammation and supporting targeted neurological rehabilitation and motor function rather than practicing mimicry and compliant behavior?
Jamison Handley, a nonspeaker and one of the authors of the book “Underestimated: An Autism Miracle” (2021) described his childhood as being in a “prison of silence” once he was able to communicate using the letterboard-based method S2C. Until he learned how to communicate using a letterboard, no one knew that he was brilliant and “stuck” inside a body that wouldn’t cooperate due to his motor-planning and execution issues.
If you haven’t seen the movie Spellers yet, I highly suggest you watch it. It will change how you view autism and nonspeakers forever. I also encourage you to check out the work of Communication4All, a nonprofit founded by Elizabeth Bonker, a nonspeaker who graduated as valedictorian from Rollins College in 2022. Elizabeth was able to excel in academics as a nonspeaker because she was given access to letterboard-based communication at a young age. Without that, Elizabeth’s motor-planning and control issues would have left her brilliant mind “trapped” inside a body that wouldn’t allow her to produce speech or reliable communication. There are young adults out there right now who have the intelligence and brilliance of valedictorian Elizabeth Bonker but are being treated everyday as if they are 3 or 4 years old due to the fact that no one has given them the opportunity to communicate with complexity and richness through a letterboard.
Children with Autism Are Being Denied the Right to Communicate
Major professional organizations that oversee the training and licensing of therapeutic professionals working with children with autism actively reject spelling methods for nonspeakers and discourage their use. ASHA (the main professional organization certifying speech and language pathologists) and leading behavior-analytic bodies, such as the Behavior Analyst Certification Board, currently discourage the use of spelling-based communication methods such as RPM, S2C, and the Spellers Method, citing lack of scientific evidence, concerns about facilitator influence, and the absence of verified independent communication. This means hundreds of thousands (and perhaps even millions) of nonspeakers are not being given the opportunity to communicate, a fundamental human right, all due to the arrogance of professional organizations that refuse to listen to testimonies of the nonspeakers themselves.
The speech-language pathologists and ABA therapists are well meaning and truly just trying to help these children improve daily function and adapt to the world around them. Most of them did not learn, and do not know, about the medical underpinnings of autism. Those speech-language pathologists and ABA therapists and technicians who do understand the medical, biological and functional root causes of the symptoms of autism are among the most valuable of professionals working with our children today. They understand the need for co-regulation. They understand that the child they are working with is coming of a place of dysregulation, overwhelm and hyperarousal. Having an awareness of these fundamental aspects of the child’s physiology can lead to completely different delivery of what could otherwise be a dysregulating therapy.
Treating the Root Causes by Focusing on Underlying Biology and Physiology
There are many paths to treating whatever may be the medical root causes or underlying dysfunctions contributing to the particular behaviors observed in autism. With regard to our earlier example of eye aversion, it is imperative that we shift our perspective from training or conditioning one to make eye contact to improving the systems that make eye contact possible and comfortable. This might include vision therapy (neuro-optometric rehabilitation) or nervous-system regulation through neurological chiropractic, vagal-nerve toning, perhaps even photobiomodulation combined with occupational therapy techniques including primitive-reflex integration. Of course, among the most important ways to improve the systems that make eye contact possible is to make the cells of the body healthy through nutrition, sunlight, movement, detoxification, and other foundational health supports.
For all symptoms and behaviors of autism, we need to address the child’s cell danger response and get their cells and their nervous system to a place where they feel safe again and where the hypervigilance can stand down. This means removing toxicants, EMFs, chronic infections (viruses, bacteria, fungi, parasites), emotional stress, artificial light, and anything else known to trigger the cell danger response. For more information on the cell danger response, please see the work of the brilliant Dr. Bob Naviaux.
Let’s look at a few of the most common “behaviors” that ABA seeks to functionally improve and instead look at the underlying biology and physiology contributing to those behaviors and what can be done alternatively from a root-causes perspective.
I’m talking about real healing here, not just symptom management or behavioral training.
In the chart below you will see the “problematic” behavior, how a BCBA might address this behavior, and in comparison, what the root cause of this behavior may be and how root causes and functionally oriented practitioners address these behaviors.
This is a symptoms-suppression/redirection approach versus a root-cause health and healing approach.
“Problematic” Autism Behavior
ABA Goal and Approach
Possible Underlying Medical/Biological Issues
Root-Cause Approach
Elopement (running away or into a dangerous situation)
Get child to respond to verbal command “stop” by providing immediate, high-value rewards (such as a favorite snack, toy) when the child responds to the word
Cell danger biology, neuro-inflammation, sympathetic nervous system activation (flight response); amygdala-driven threat detection; poor interoception; sensory avoidance
Get the nervous system into a more regulated state through: coregulation, neurological chiropractic, vagal-nerve toning, reflex integration; establish cellular, mitochondrial, & metabolic health through natural rhythms, detoxification and nutrition; reduce brain inflammation through detoxification, microbiome support and immune system regulation
Lack of functional communication
Replace frustration or behaviors with gestures of communication to express wants and needs; encourage words or gestures to communicate needs; reward words and gestures used appropriately
Whole-body motor dysfunction, atypical development /mitochondrial dysfunction in Broca’s/Wernicke’s areas; motor-planning issues; auditory-processing differences, brain inflammation that precipitates sensory challenges and difficulty decoding spoken language in real time
Establish cellular, mitochondrial, & metabolic health through natural rhythms, detoxification and nutrition, nervous-system regulation through neurological chiropractic, vagal-nerve toning, reflex integration; reduce brain inflammation through detoxification, microbiome and immune system regulation; re-establish motor function through OT and targeted manual-motor therapies; rehabilitate regions of low mitochondrial function through OT and photobiomodulation;
Anger, harmful or aggressive behaviors. Self-injury (head banging, biting); aggression; severe tantrums
Nervous system is producing a survival response; amygdala hyper-reactivity/ (threat detection system overfires); ANS dysregulation—sympathetic dominance (“fight/flight”); neuroinflammation; pain; sensory overload; low inhibitory control (prefrontal cortex mitochondrial dysfunction)
Notice that the “root-cause approach” for all of these seemingly disparate symptoms is kind of the same. Each of the symptoms can be treated by getting the nervous system into a more regulated state, establishing cellular, mitochondrial, and metabolic health, reducing brain inflammation and treating areas of the brain that need additional rehabilitation or mitochondrial support with targeted therapeutics.
Sounds like a lot, doesn’t it? It is, and it isn’t. Conceptually, it’s simple. This is about shifting the body into a healing state. When overwhelming obstacles to healing (toxins, infections, stress, EMF) are present, the body can never fully shift into a healing and repairing state. When those obstacles are removed, the body knows how to heal. It wants to heal.
Practically speaking, getting a severely dysregulated child’s body into a healing state can be incredibly challenging. It requires changing your diet, your activities, your living environment, your mindset. Everything.
While each individual child may need specific individualized therapeutic rehabilitative supports (such as photobiomodulation or neuro-sensory-motor rehabilitation), the body cannot overcome this state of dysregulation without foundational health supports: nutrition, sleep, movement, oxygenation, hydration, sunlight, nature. Those are the non-negotiables. But they are also the healing modalities that are the least expensive and most accessible.
These “simple” foundations may not be easy for a family that has a child who is so dysregulated that removing an iPad can be a life-threatening act. But imagine if we made these foundations the priority. Imagine if we committed just 20 hours a week to supporting the health of the cells and the nervous system instead of committing to 40 hours a week to repetitive tasks in an indoor gym-like setting surrounded by (often toxic) foam mats, plastic balls, fluorescent lights and people who don’t necessarily presume that your child is brilliant but trapped in an apraxic body.
The root-cause approach shifts the focus from managing or redirecting behaviors through therapy to assessing and addressing underlying medical and physiological imbalances and dysfunctions. Healthy cells and systems are the precursors to regulated behavior. Remember, most children with autism are living in a state of chronic danger biology. The behaviors are a direct reflection of that.
Re-Imagining Autism Care
Let’s imagine what it would look like (and what it would cost) if we chose to use a root-cause model for treating autism instead of the behavioral-management model of ABA.
Twenty hours of ABA for a child with moderate to severe autism will cost between $1,300-$4,000 per week, with an average of about $2,400. This is literally what is being billed to Medicaid and private insurance every week. Let’s assume this ABA program occurs for 40 out of the 52 weeks in a year. That equates to $96,000 a year in ABA service fees. (Your tax dollars and insurance premiums at work.)
Let’s do the intellectual exercise of pretending that a root-cause functional and medical approach to treating autism were covered by insurance and Medicaid.
What type of care might a child with moderate-to-severe autism receive in this scenario (and how much would it cost) per year? A root-cause therapeutic program for a child would be bioindividualized, so this program really can’t be extrapolated to every child, but let’s assume we are talking about a hypothetical child with level 2 autism who has been assessed to need the following:
- Parent education program to teach parents how to reduce total load of health stressors, how to cook nutrient-dense meals to support the child’s overall metabolic and cellular health, and how to establish regulating rhythms and practices in the home (sleep, no screens, nature and sunlight exposure). This would require about 20 hours of education at a cost of about $800 total.
- A neurological chiropractor for nervous-system regulation. Estimate two or three 10-minute visits per week, plus additional “homework” of nervous-system regulation practice (vagal toning, breathing, coregulation between parent and child). This would require about 30 minutes a week for 40 weeks for a total of 20 hours in a year at a cost of $4,800.
- Functional medical doctor, functional nutritionist, or other natural health practitioner to support laboratory diagnostics, medical care, and nutritional guidance to pinpoint ways to improve cellular health, reduce inflammation, support mitochondrial health, treat chronic infections, restore the microbiome. This would require about 12 hours of time at a cost of $8,400 for a year. (Lab tests at $3,000; practitioner fees at $3,000; supplements and medications at $2,400/year).
- Rehabilitative work, if needed, would include one or more of the following types of therapies: reflex integration, speech therapy, photobiomodulation, brain-body integration therapies, vision therapy, auditory-integration therapy, occupational therapy, etc. This would require about 120 hours in a year at a cost of about $18,000 ($150/hour, 3x a week for 40 weeks).
- A health coach to help the family navigate diet and lifestyle changes required to restore cellular health—This would require 20 one-hour sessions ($100/hr) at a cost of $2,000.
- For nonspeakers, supporting communication needs (spelling) while treating the underlying motor dysfunction may require additional support such as Spellers Method training for a parent or caregiver. Estimate $3,000-$6,000.
Using this hypothetical scenario, the total commitment for this type of treatment for one year would be:
ABA => $96,000, requiring 800 hours
Root-Cause Approach => $34,000 requiring 192 hours
Below is the breakdown of the hours and costs in the two different types of approaches, ABA vs. a root-cause functional and medical approach:
ABA Hours
ABA Cost
Root-Cause Hours
Root-Cause Cost
Parent-Education Program
20
$800
Nervous-System Regulation Clinician
20
$4,800
Functional Medicine-Clinician, Testing and Treatment
12
$8,400
Health Coaching
20
$2,000
ABA Therapist
800
$96,000
TOTAL
800
$96,000
192
$34,000*
*Add an additional $3,000-$6,000 if needing spelling or communication method training/practitioner.
While the root-cause approach requires more types of modalities and interventions, it is about a third of the cost of the ABA-only approach and requires less than one quarter of the time commitment. The best part about the root-cause approach is that some of the children may actually overcome their diagnosis as a result. You read that right. They may no longer qualify for an autism diagnosis after this kind of care and treatment. (See the section on Peer-Reviewed Documentation of the Reversal or Remission of Autism Symptoms and/or Diagnosis below for documentation of autism symptom reversal/recovery resulting from these types of interventions.)
The average ABA program recommends that the child stay enrolled in ABA for 3-5 years. Let’s do the math on that. The total spend on ABA for one child will range from $288,000-$480,000, whereas the intensive root-cause medical treatment may only be needed for 1-3 years (depending on severity of the child’s case) at a total cost of between $34,000-$102,000, and the outcomes are likely to be far better.
What’s more, if the root-cause medical approach is applied early (while a child is under 3 years old), some of those costly “rehabilitative” type therapies may never be needed!
The root-cause medical and functional approach costs a fraction of the ABA approach, requires a fraction of the time commitment, and in some cases, results in full reversal or loss of diagnosis.
ABA: Very Expensive, Very Covered
Parents, this is the part where you need to start getting angry.
Why does ABA persist as the dominant therapy and treatment for children with autism, despite the fact that a root-cause holistic and functional-medical approach results in far better outcomes and is a fraction of the price and time commitment?
ABA is done one-on-one, which means it is a very expensive and labor-intensive form of therapy. It takes hours and hours of repetitive tasks led by a BCBA or RBT to accomplish the goals of treatment. Therapy typically costs between $120 to $200 per hour when billed to private insurance and $65-$130 per hour when billed to Medicaid. Interestingly, the average BCBA makes between $30 and $65 an hour, a technician may make less than that, so there is a lot of overhead and profit-making going on here.
If we are being conservative and estimating that a child is only receiving 10 hours of ABA per week, it would still cost between $36,400 and $104,000 per year (depending on whether it is billed to private insurance or Medicaid).
This is an outrageous and unsustainable cost to parents, to taxpayers, and to insurance companies and their premium payers. Many children with autism are prescribed up to 40 hours of ABA per week and 20-40 hours per week is considered the norm for “intensive” therapy for children who are diagnosed with level 3 or severe autism. Forty-hours per week of ABA therapy is somewhere between $145,000 (low end Medicaid reimbursement) and $416,000 (high end, private insurance reimbursement).
Nearly half a million dollars per year per child with severe autism?? How did we get here?
How ABA Came to Be Covered (and Why You Can’t Get Coverage for Root-Cause Treatments or Functional Medicine)
If you ask developmental pediatricians, psychiatrists or others who diagnose autism why ABA is so widely covered, they will tell you that it is because it is the “gold standard” and only “evidence-based” treatment for autism.
Starting in the 1960s, behavioral psychologists began studying ABA as a possible therapy for autism (it was not developed for autism; it was an existing behavioral psychology modality applied to autism). This research led to the collection of evidence by researchers (really expanding with Ivar Lovaas at UCLA in the 1980s) demonstrating that ABA resulted in meaningful behavioral change in children with autism. Subsequently, hundreds of ABA studies have been conducted in children and adults with autism where it has been shown to be “effective.” But what does “effective” actually mean?
“Effective” does not mean “cures autism,” or “reverses the symptoms of autism”, or “treats the underlying physiological imbalances or developmental dysfunction,” and it usually does not mean “produces broad, proven improvements in quality of life.”
In the ABA literature, “effective” usually means that, compared with no treatment, or random eclectic services, children showed improvement on researcher-selected measurable outcomes such as IQ/cognitive scores, adaptive behavior, language/communication, daily-living skills, and sometimes reduction in certain challenging behaviors or autism-severity ratings. ABA is “effective” and “evidence-based,” but remember, it is forcing behavior out of children who can’t do the behaviors or who feel unsafe when doing so.
In 1999, the U.S. Surgeon General published a report endorsing applied behavioral methods for autism. Then in 2001, a National Research Council report titled Educating Children with Autism gave behavioral intervention a central place in early treatment discussions. Finally, pediatric and specialty guidance over time helped normalize referral to behavioral intervention early in life. Together, those endorsements made ABA look like the most “official” autism treatment in the policy world.
Enter Autism Speaks
The real action happened when Autism Speaks, founded in 2005 by the wealthy and well-connected Bob and Suzanne Wright, launched an initiative to get autism services covered. Bob Wright was the Former CEO/Chairman of NBC Universal whose grandson, Christian, was diagnosed with autism in the early 2000s. At the time there was very little in the way of awareness or support for families with children with autism. The Wrights and Autism Speaks raised tens of millions of dollars each year for autism, and a good portion of that funding went to a multi-year, 50-state initiative to get ABA therapy covered for autism.
ABA became covered by Medicaid and private insurers because Autism Speaks orchestrated a coordinated, professionally run, multi-year, multi-million-dollar national policy campaign in state legislatures across the country. This campaign started in 2005 and continued right up until the last state acquiesced in 2017. It was truly a herculean effort.
IRS Form 990 filings show that Autism Speaks has typically generated tens of millions in annual revenue since 2005, peaking near $100 million per year and more recently averaging around $30–40 million per year. This money was necessary to shift policy in favor of supporting covered services for autism, but these services do not include biomedical, functional or root-cause services—just ABA, and some speech and occupational therapy.
In 2014, CMS (Centers for Medicare & Medicaid Services) issued a bulletin that clarified that Medicaid must, by law, cover “medically necessary” treatment for autism. Autism Speaks and allied advocacy organizations had already pushed legislation forward in most states to establish that ABA was medically necessary. This CMS bulletin essentially removed any legal gray area around whether or not ABA had to be covered by Medicaid. From a business standpoint, this Medicaid bulletin and the legislation that had been passed in nearly every state meant that an ABA services business could expect reliable income, both from private insurers and from Medicaid. It was now the law. This caught the attention of investors, particularly private equity.
Check out the chart below. You can see by looking at the dotted line that insurance reform in each of the states profiled resulted in massive growth in BCBA, BCBA-D and BCaBA (ABA therapists) certification.
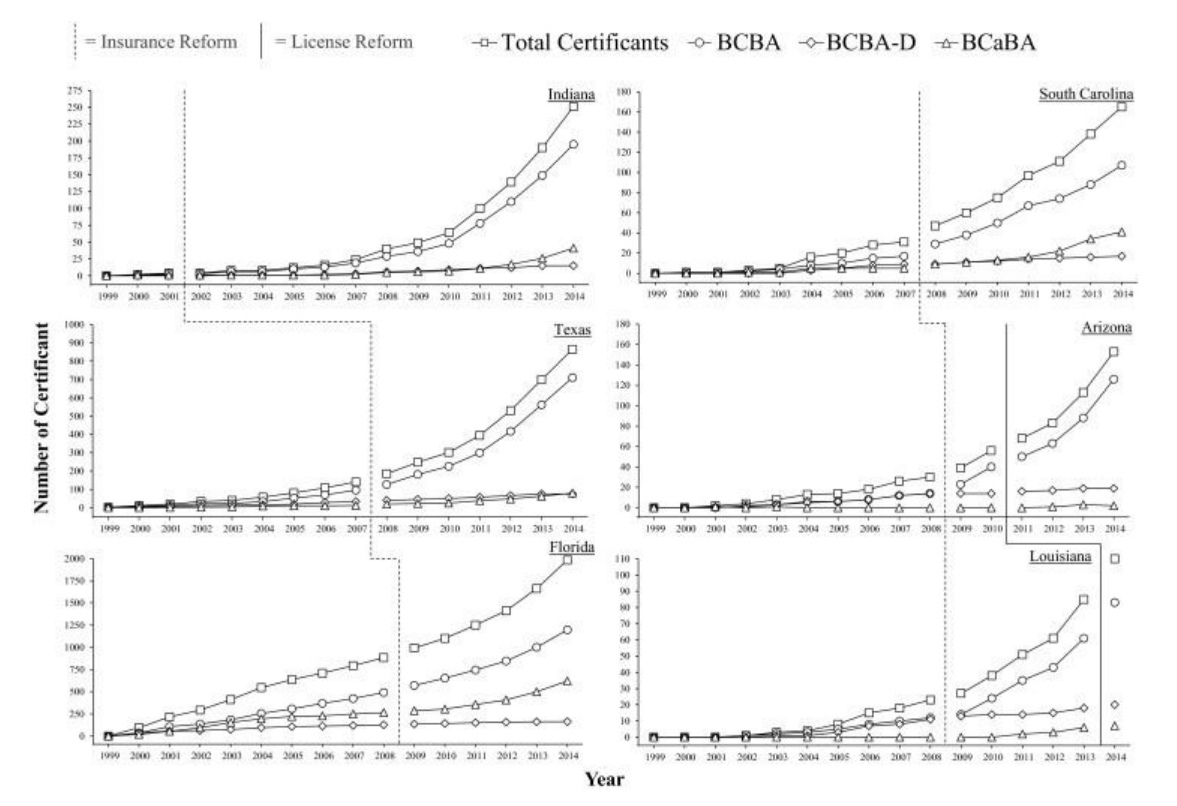
Source: BACB Certification Trends: State of the States (1999 to 2014), available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC4999363/
Enter Private Equity
Once payment for ABA services had been codified into law, and the rates of autism continued to grow dramatically every year, autism evolved from a niche “genetic” condition into a “market opportunity.” Suddenly, investors saw the business case for rolling up ABA centers and turning them into profit centers. This is how ABA scaled so rapidly.
It isn’t until around 2014 that autism and autism therapy (ABA specifically) started appearing alongside words like “market” or “investment opportunity”. You can search the wayback machine (internet archives) to find some of the earliest “autism investment” meetings and conversations and they don’t really appear until 2014 or later. By 2019, autism was routinely referred to this way. Today, you will commonly see asset-management companies and investment professionals talk about autism therapy as an “active area for investment,” or a “growth market.”
L.E.K. Consulting, a global strategy consulting firm, has estimated that the U.S. ABA therapy market is soon projected to be a $25-$35 billion market with a 10-13% annual growth rate. In their 2025 Autism Therapy Market Trends Report, they encourage their investor clients to seize on this favorable investment opportunity due to anticipated growth and reliable payor infrastructure (Medicaid and insurance mandates).
Investors are looking for high-demand, under-supplied, reimbursement-backed services that can be standardized and scaled. And the ABA therapy market is answering that call.
Cha-ching!
A 2023 report published by the Center for Economic Policy and Research titled “Pocketing Money Meant for Kids: Private Equity in Autism Services,” raises the alarm bells about the potential for exploitation of children with special needs due to market dynamics. This report details how between 2017 and 2022, private equity firms like Black Stone aggressively began consolidating the market, buying up private clinics, capturing efficiencies, and maximizing profits. Most objective observers will argue that this has come at the expense of care quality, workforce conditions, and equitable access.
One indicator of the low quality of care and poor workforce conditions (a signature of private equity takeovers!) is the high turnover rate among ABA therapists and technicians. The turnover rate of RBTs in ABA therapy centers ranges from 65% to 100% turnover rate annually. Think about this! In some ABA therapy centers, especially the larger ones owned by private equity, the lower paid RBT technicians are quitting before they even complete one year of employment!
This is a churn-and-burn business, baby!
While the ABA “market” is currently estimated to generate nearly $8 billion in revenues annually, investors see the opportunity for it to grow to tens of billions annually because the demand is so high (because we have so many sick kids!!).
The most alarming part of private equity entering the autism therapy market is that the money that is required to pay for this very expensive and intensive treatment isn’t used to optimize high quality care for children with autism. It is diverted to executive compensation and returned to private equity investors. Private equity currently owns hundreds of ABA clinics (574 sites across 42 states as of 2024) and this type of ownership is also more likely in states where there are more generous autism insurance mandates. This is a clear reflection of market forces at play.
What may have started as a philanthropic and social enterprise by Bob and Suzanne Wright has morphed into an exploitative market-driven trainwreck. And autism families are left with few other choices.
[Side note: fraudsters and criminals are actively getting in on the perceived cash cow of government-funded autism services. And they are taking full advantage of you and your tax dollars, to the tune of hundreds of millions of dollars stolen from the government in fraud schemes. Are we angry yet?]
Private equity may have gotten away with this while the numbers of children with autism were under 1%, but we are now at least at 3.2% of children and growing. This will bankrupt insurers and state health insurance agencies (not to mention the strain on IDEA and state and local education budgets). Do not misunderstand me. I am not advocating for taking away any services for your child. I am advocating for prioritizing those dollars to medical services that address the underlying physiological imbalances precipitating the behaviors that we label autism. ABA can still be utilized and can be helpful, but I believe it should be implemented only after a child’s primary medical needs are met. Let’s get their bodies healthy and regulated and then we can work on the behavior.
If ABA Is Considered “Medically Necessary,” and Covered by Medicaid and Private Insurance, Shouldn’t Functional-Medical Treatment of Autism Also Be Covered?
Ironically, while a behavioral therapy is widely covered, actual medical treatment of autism, including functional medicine, nutritional intervention, neuro-optometry, neurological chiropractic, and other treatments aimed at correcting medical and physiological imbalances in children are not covered.
A comic strip of a child and a doctor AI-generated content may be incorrect. Are we in bizarro world? Behavioral treatment is deemed “medically necessary” but actual medical treatment is not considered medically necessary? Okay, got it.

Reprinted with permission of Martin Matthews.
Much of this has to do with the fact that the medical establishment refuses to acknowledge that autism is a medical condition. Despite the fact that parents have tried for decades to get treatment for the clear medical issues that their children are dealing with, the medical concerns are often dismissed as “just a part of autism.”
This gaslighting of parents persists despite the fact that there are thousands of papers published in the peer-reviewed medical literature exploring the biological and physiological mechanisms that precipitate behavioral symptoms in autism. You can find many of these papers in the sources and references section of this article, and this article, as well as in the Autism Knowledge Gateway, a comprehensive library of autism biomedical literature.
Peer-Reviewed Documentation of the Reversal or Remission of Autism Symptoms and/or Diagnosis
Dr. Deborah Fein at the University of Connecticut has been tracking what she terms “Loss of Autism Diagnosis,” or LAD, for well over a decade. In a 2023 editorial paper published in the Journal of Child Psychology and Psychiatry, Fein and colleagues summarize years of research documenting dozens of cases of individuals who met the criteria for autism in childhood who no longer qualified for this diagnosis over time or into adulthood. Dr. Fein and her colleague Inge-Marie Eigsti acknowledge the challenge this type of research presents, as many people believe that autism is a neurotype that cannot be changed. Dr. Eigsti and colleagues argue that loss of autism diagnosis is real and needs to be better understood, and we cannot dismiss what has been objectively observed just because autism is interwoven with issues of identity. In 2018, Dr. Fein and colleagues won a $3 million NIH grant to study this phenomenon. You do not win a $3 million grant from the NIH if what you are studying isn’t real or based in evidence.
Furthermore, there are a number of case reports in the medical literature describing the reversal or remission of autism symptoms and even complete loss of an autism diagnosis through bioindividual medical treatment. Here are just a few of those papers:
- 2008: O’Hara and Szakacs documented the case of an autism recovery achieved through personalized biomedical interventions
- 2013: Herbert and Buckley described a child whose autism severity score dropped from severe to non-autistic and her intelligence quotient increased by 70 points following dietary intervention
- 2016: Grossi and colleagues reported improvement in core autism symptoms following probiotic treatment in a child with gastrointestinal dysfunction
- 2020: Baker and Shaw reported a case of complete recovery from autism after treating a suspected Aspergillus fungal overgrowth with antifungal medication
- 2023: Offutt and Breitschwerdt reported substantial improvement in cognitive and neurobehavioral symptoms following treatment of vector-borne infections
- 2024: D’Adamo and colleagues documented reversal of autism symptoms in twin toddlers using a personalized approach that included diet, environmental modification, and targeted medical support
Biomedical and “root-cause” assessment and treatment of autism are not deemed “medically necessary” by Medicaid and insurance companies because policy hasn’t caught up with the science yet. In public-health conversations, autism is still framed as a genetic behavioral/developmental condition, rather than a medical condition marked by quantifiable medical issues (mitochondrial dysfunction, metabolic impairments and disease, cellular toxicity, microbiome perturbations and inflammatory bowel disease, autoimmunity, nutritional deficiencies, cerebral folate deficiency, autonomic nervous system dysfunction, among other treatable medical issues). Most clinicians call these “co-morbidities” as if the autism caused the medical issues. It is the other way around: the underlying medical issues are the problem, and the behavioral symptoms of autism are the “co-morbidities.” When you treat the medical problems, many, if not all, of the behavioral problems go away.
Under EPSDT (Early and Periodic Screening, Diagnostic, and Treatment, an important Medicaid benefit), children are entitled to all 1905(a) coverable, appropriate, and medically necessary services needed to “correct or ameliorate” their conditions. Section 1905(a) includes services such as:
- Physician services
- Hospital services
- Laboratory and X-ray services
- Home health services
- Early and Periodic Screening, Diagnostic, and Treatment (EPSDT)
- Physical therapy, occupational therapy, speech therapy
- “Other licensed practitioner” services
- Rehabilitation services
- Case management
- Prescription drugs
Here’s the catch: state Medicaid agencies and private insurers get to decide what services are deemed “medically necessary,” so they may deem treatment with Risperdal (a pharmaceutical with a horrific side-effect profile) a “medical necessity,” but functional nutritional therapy aimed at restoring a healthy microbiome, mitochondrial function and metabolic balance for a child with autism is not considered “medically necessary.” Make that one make sense.
There is a very strong argument to be made that functional and medical treatment of autism is “medically necessary.” But when you dig into what is required to demonstrate its necessity, you meet the same barrier over and over again. The system requires that you provide high quality evidence demonstrating that functional and medical treatment of autism results in better outcomes than the current standard of care (basically, ABA). In our reductionist western medical model, this generally means we need to produce randomized controlled trials demonstrating that functional-medicine testing (like organic acids tests, microbiome tests, toxicity testing, infection testing, etc.) and functional treatment (targeted nutrition, detoxification strategies, nervous system regulation, etc.) result in significantly improved outcomes for children with autism. So how do we do that type of trial?
Once you get into setting up the study design, you realize that institutional science wants to see standardization – the same set of labs paired with the same interventions that can both be measured against outcomes. Herein lies the rub. There is no standardization in autism. Because autism is so bio-individual, it is nearly impossible to run gold-standard clinical trials testing biomedical therapeutic interventions. Each child needs an individualized set of assessments (based on a detailed clinical history) and an individualized and adaptive intervention plan.
What Will It Take to Get Coverage for Root-Cause Medical Treatment of Autism?
For payers, the question is not always, “Is there a perfect randomized controlled trial?” It is often, “Is there enough reliable evidence to justify coverage for this subgroup, and can we monitor results?” There is one possible way to gather this level of evidence. Practice-based registries are an acceptable way to gather outcomes evidence while respecting the variability in assessments and treatments. The FDA, institutional review boards and medical authorities are increasingly recognizing real-world evidence as clinically meaningful when the data are relevant and reliable.
Essentially, we need a robust registry-style autism study that will show that enrolled children with autism have documentable, treatable medical problems that, when addressed, experience significant functional improvements. Another way to say this is that some children diagnosed with autism also have remediable metabolic, gastrointestinal, infectious, immune, nutritional, toxicant-related, and sleep-related contributors to functional impairment; identifying and treating those contributors can improve communication, behavior, adaptive function, GI symptoms, sleep, and quality of life. A sufficiently powered registry study designed to assess functional improvements in children receiving medical treatment might be our best shot at getting coverage.
The Autism Moonshot: The Policy Can Be Changed, But It Won’t Be Easy
Following is a step-by-step plan for shifting policy with regard to autism and our payor system.
Step 1: Create a prospective registry
This would require enrolling children into a prospective (looking forward) registry across functional medicine clinics in the U.S. at diagnosis. The clinics would need to use a common data model, prespecified inclusion criteria, and standardized follow-up intervals. [At present, no one is pursuing this type of study. If Documenting Hope had sufficient funding, we would be thrilled to run this study. Please contact me if you, or someone you know, wants to fund it!]
Step 2: Ensure that there is a pragmatic comparison model included in the study
Compare “usual autism specialty care” (ABA) versus “usual care plus root-cause pathway” in real-world clinics. Some data and outcomes that could be tracked include:
- Adaptive function
- Communication function
- Sleep
- GI symptom burden
- Irritability/self-injury/elopement frequency
- Parent-reported quality of life and caregiving burden
- ER visits, hospitalizations, psychotropic use, constipation meds, sleep meds
These are not “autism severity” metrics, these are functional-improvement metrics, which would be required to demonstrate improvement in function (the threshold for proving “medical necessity” because the existing standard of care is measured this way) and to have metrics that compare nicely with the outcomes measured in ABA.
Step 3: Publish results from the prospective registry in peer-reviewed literature and encourage peers to replicate.
To move the needle on the payor side of things, any improvements in function need to exceed what is already documented with regard to ABA outcomes and the findings also need to be replicated in at least one other large study.
Step 4: Bring this evidence to the state Medicaid agencies and private insurers
Just as happened earlier in the 2000s under the leadership of Autism Speaks, state legislators need to be convinced of the medical necessity of providing functional and root-cause medical treatment to children with autism. These published registries would be the first step, but then the lobbying needs to begin. Once this evidence has been established, coverage could be requested for targeted evaluation and management of documented medical problems contributing to functional impairment in children with autism. We would need an Autism-Speaks level, 50-state initiative to educate legislators on the medical necessity of this type of treatment.
According to their federal 990, Autism Speaks had $35 million in assets in 2024. Perhaps they might like to throw some of that sweet cash towards this type of study?
Here is their phone number in case anyone wanted to call them to suggest this idea: (202)-955-3111.
Short of This Autism Moonshot, Can We Get Any of These Services Covered??
The lowest-hanging fruit right now is to study outcomes related to parent-led interventions, things you can do at home, with support from a knowledgeable autism coach.
CMS (Medicaid) just recently created a CPT code (a code used for billing and insurance) covering health coaching, so it’s reasonable to think that we might get autism coaching covered in the near future.
To get Medicaid to cover this type of support, it would need to be framed as a clinician-supervised, caregiver-mediated intervention that improves medical outcomes and functional status. And there would need to be data supporting improved outcomes in families that utilized health coaching.
Luckily, Documenting Hope is currently running an IRB-approved study right now to test outcomes of a parent-education and coaching program for autism. It is called the FLIGHT-Autism Study. We are studying the impact of a structured education and coaching program on functional outcomes in children with autism. Stay tuned for updates from that study!
Until We Make These Changes to the Payor System, How Will I Afford Biomedical Treatment for My Child?
While functional-lab testing and medical and root-cause treatment of autism by clinical professionals can certainly accelerate and expedite the healing, a lot of the healing work can be done at home with parent-led initiatives.
If you really want to help your child heal and regulate, you need to make a commitment to making every feasible diet and lifestyle change you can. I’ve been tracking stories of families that have reversed autism for nearly 20 years. Not one of them had healing success without doing a complete overhaul to their diet and lifestyle. If that sounds intimidating, please know that you do not have to do this alone. Documenting Hope is here to support you. You can join our community of parents walking this path together, here.
It’s okay if you sit on your kitchen floor crying and screaming every morning because you are trying to do the right thing by feeding your child healthy, nutritious food, but your child won’t eat anything. It’s okay that you feel confused and overwhelmed because you don’t know what to do next. Lots of parents have sat in that exact same spot on the kitchen floor. Crying. Angry. Grieving.
But you will pick yourself up and you will put one foot in front of the other, and you will do what you need to do and learn what you need to learn to help your child begin to heal. Do you know how I know this? Because our team at Documenting Hope has seen hundreds of parents just like you figure out exactly what their children needed to heal. And you will, too. Your child and your family are worth it.
And while you are putting one step in front of the other on your family’s healing journey, we’ll be right there with you. We can’t make breakfast that your child with ARFID will eat; we can’t help you collect the urine and stool samples to ship off for root-cause testing; and we can’t make the phone call for you to get in see the functional practitioner that is in your community. But what we can do is this:
- Continue to write articles, ebooks, create content, and host interviews with experts to provide you with the latest information that may be relevant to your child’s healing journey
- Show up for you and every other member of Healing Together to listen to your stories and answer your questions live in our membership community
- Host a comprehensive directory of professionals who are your boots-on-the-ground helpers for families in communities around the world
- Train more health coaches to be ready to assist you when you need them
- Host educational conferences and events to give everyone in our healing community a chance to learn from the experts and share healing stories and strategies
- Continue to pursue and publish independent research to build the body of evidence that autism is preventable and reversible in many cases.
Documenting Hope will continue to offer this support because we love your children and we believe in their future. And we believe in you, too.
About Beth Lambert
Beth Lambert is a former healthcare consultant and teacher. As a consultant, she worked with pharmaceutical, medical device, diagnostic and other health care companies to evaluate industry trends.
She is the author of A Compromised Generation: The Epidemic of Chronic Illness in America’s Children (Sentient Publications, 2010). She is also a co-author of Documenting Hope's Brain Under Attack: A Resource for Parents and Caregivers of Children with PANS, PANDAS, and Autoimmune Encephalitis. She is a co-author of Reversal of Autism Symptoms among Dizygotic Twins through a Personalized Lifestyle and Environmental Modification Approach: A Case Report and Review of the Literature, J. Pers. Med. 2024, 14(6), 641.

In 2009, Beth founded Documenting Hope and currently serves as Executive Director. Beth attended Oxford University, graduated from Williams College and holds a Masters Degree in American Studies from Fairfield University.
Still Looking for Answers?
Visit the Documenting Hope Practitioner Directory to find a practitioner near you.
Join us inside our online membership community for parents, Healing Together, where you’ll find even more healing resources, expert guidance, and a community to support you every step of your child’s healing journey.
Sources & References
Akkaş, Ö., et al. Ophthalmological Findings and Their Clinical Correlations in Children With Autism Spectrum Disorder: A Comparative Study. Int J Psychiatry Med. 2026 Feb 9:912174261425404.
Baker, S., et al. Case Study: Rapid Complete Recovery From An Autism Spectrum Disorder After Treatment of Aspergillus With The Antifungal Drugs Itraconazole And Sporanox. Integr Med (Encinitas). 2020 Aug;19(4):20-27.
Bemporad, J.R. Adult recollections of a formerly autistic child. J Autism Dev Disord. 1979 Jun;9(2):179-97.
Bharath, R., et al. Comparison of Physiological and Biochemical Autonomic Indices in Children with and without Autism Spectrum Disorders. Medicina (Kaunas). 2019 Jul 7;55(7):346.
Chiu, H.T., et al. Resting Heart Rate Variability and Emotion Dysregulation in Adolescents with Autism Spectrum Disorder. J Autism Dev Disord. 2024 Apr;54(4):1482-1493.
D’Adamo, C.R., et al. Reversal of Autism Symptoms among Dizygotic Twins through a Personalized Lifestyle and Environmental Modification Approach: A Case Report and Review of the Literature. J Pers Med. 2024 Jun 15;14(6):641.
Deochand, N., et al. BACB Certification Trends: State of the States (1999 to 2014). Behav Anal Pract. 2016 Mar 28;9(3):243-52.
Eigsti, I.M., et al. Editorial Perspective: Another look at ‘optimal outcome’ in autism spectrum disorder. J Child Psychol Psychiatry. 2023 Feb;64(2):332-334.
Gazjago, G., et al. Two cases of “recovery” in Kanner syndrome. Arch Gen Psychiatry. 1974 Aug;31(2):264-8.
Grossi, E., et al. Unexpected improvement in core autism spectrum disorder symptoms after long-term treatment with probiotics. SAGE Open Med Case Rep. 2016 Aug 26:4:2050313X16666231.
Herbert, M.R., et al. Autism and dietary therapy: case report and review of the literature. J Child Neurol. 2013 Aug;28(8):975-82.
Knight, E.J., et al. Severely Attenuated Visual Feedback Processing in Children on the Autism Spectrum. J Neurosci. 2023 Mar 29;43(13):2424-2438.
Matta, S.M., et al. The influence of neuroinflammation in Autism Spectrum Disorder. Brain Behav Immun. 2019 Jul:79:75-90.
Naviaux, R.K. Metabolic features of the cell danger response. Mitochondrion. 2014 May:16:7-17.
Naviaux, R.K. Perspective: Cell danger response Biology-The new science that connects environmental health with mitochondria and the rising tide of chronic illness. Mitochondrion. 2020 Mar:51:40-45.
Offutt, A., et al. Case report: Substantial improvement of autism spectrum disorder in a child with learning disabilities in conjunction with treatment for poly-microbial vector borne infections. Front Psychiatry. 2023 Aug 18:14:1205545.
O’Hara, N.H., et al. The recovery of a child with autism spectrum disorder through biomedical interventions. Altern Ther Health Med. 2008 Nov-Dec;14(6):42-4.
Price, A., et al. Understanding the subtypes of visual hypersensitivity: Four coherent factors and their measurement with the Cardiff Hypersensitivity Scale (CHYPS). Vision Res. 2025 Aug:233:108610.
Stuart, N., et al. Eye Gaze in Autism Spectrum Disorder: A Review of Neural Evidence for the Eye Avoidance Hypothesis. J Autism Dev Disord. 2023 May;53(5):1884-1905.
Tottenham, N., et al. Elevated amygdala response to faces and gaze aversion in autism spectrum disorder. Soc Cogn Affect Neurosci. 2014 Jan;9(1):106-17.








